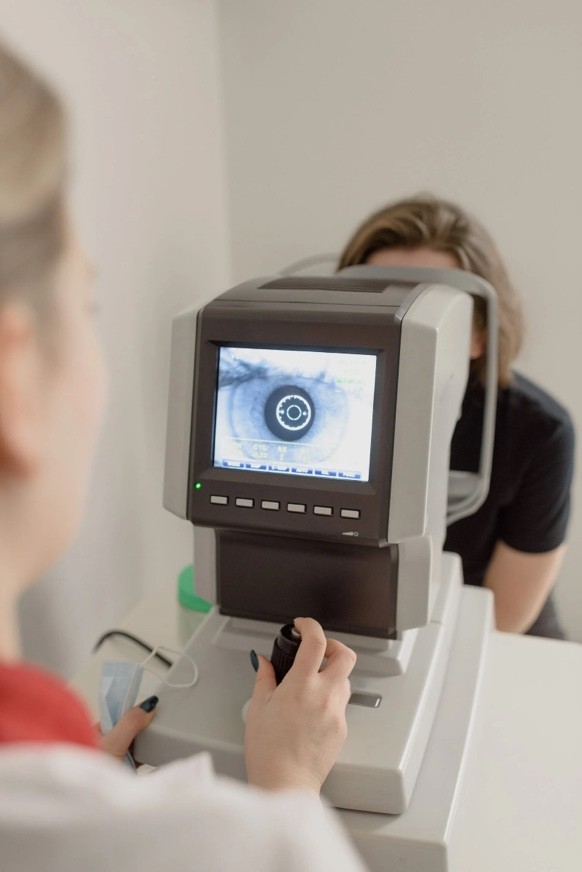
It involves the study of the structure, function, and diseases of the eye and its associated structures, including the eyelids, conjunctiva, cornea, iris, lens, retina, optic nerve, and the surrounding tissues.
General ophthalmologists provide comprehensive eye care services, including: